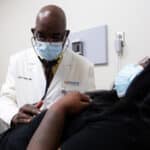
If your clients are baby boomers, they are part of a group that’s drinking longer and abusing alcohol in greater numbers than previous generations.
Among those old enough to remember using marijuana as a statement against authority, its legalization has inspired rising abuse and the danger of acute intoxication.
A significant number taking opioids for pain relief are also mixing drugs with other medicines and alcohol to a greater, more dangerous degree than ever.
And some elderly insomniacs say they can’t imagine life without taking sleeping pills.
According to the keynote speaker at a recent webinar on substance-use disorders, substance abuse among older patients “must be paid attention to and needs much more study,’’ said Frederic C. Blow, director of the University of Michigan Addiction Center (https://medicine.umich.edu/dept/psychiatry/programs/addiction-center).
Blow spoke at the fourth annual Older Adult Mental Health Awareness Day Symposium held recently by the National Council on Aging, the U.S. Administration for Community Living and the Substance Abuse and Mental Health Services Administration, SAMHSA. Eric Weakley of SAMHSA moderated.
Warning Signs and Causes
Common signs of substance disorder include diminished psychomotor performance, impaired reaction time, loss of coordination, falls, daytime drowsiness, and confusion and aggravation of emotional states.
Blow said that, according to SAMHSA, “abuse of alcohol and prescription drugs among adults 60 and older is one of the fastest-growing health problems facing this country; in the United States, it is estimated that 2.5 million older adults have problems related to alcohol, and adults age 65 and older consume more prescribed and over-the-counter medications than any other group.’’
Moreover, “problems stemming from alcohol consumption, including interactions of alcohol with prescribed and over-the-counter drugs, far outnumber any other substance abuse problem among older adults. Many over-the-counter drugs negatively interact with other medications and alcohol.’’ Blow said that although his own physician is now counseling and screening his patients about substance abuse, many doctors still do not.
“We recommend that all those who are 60-plus have a yearly screening for substance abuse,’’ Blow said.
Causes of substance disorder in older people include loss of spouse, friends, family members; retirement; social isolation and loneliness; loss of physical attractiveness; declining health; and problems in managing leisure time.
In screening older patients for alcohol abuse, Blow said that clinicians “should talk (to their patients) about the nature and extent of the problem in later life and the risks and benefits of alcohol use.’’
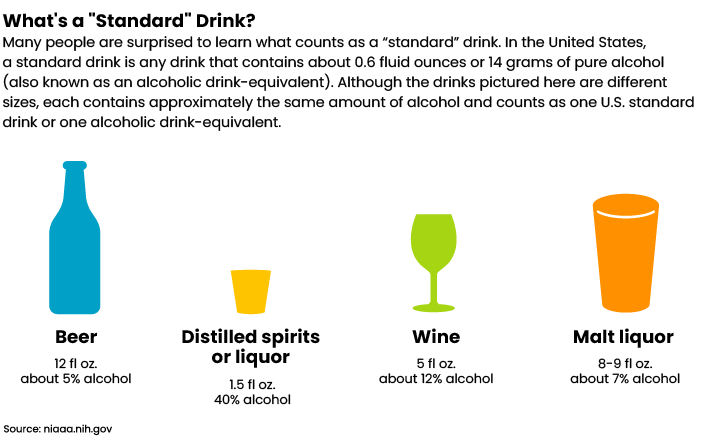
By the Numbers
According to the National Institutes of Health, a standard drink is as follows: 5 ounces of 12% wine; 1.5 ounces 40% (80 proof) distilled spirits or liquor; 12 ounces of 5% beer and 8 ounces of 7% malt liquor.
SAMHSA says one drink per day is appropriate for males 65 and older, with slightly less than that for women.
“Low to moderate drinking on a daily basis can help heart health, and there is the social aspect,’’ Blow said.
“But, hundreds of studies show that the risks can include gastritis, ulcers, liver and pancreas disease, gout, breast cancer, hypertension and diabetes, and more,’’ he said.
Drinking in older people can be “a surrogate for nutrition and exercise,’’ and can “cause depression and anxiety,’’ Blow said.
In response to increasing overdoses among opioid users, the Biden Administration recently announced that opioid overdose deaths hit their highest point in a 12-month period ending September 2020, with more than 97,000 deaths.
A total of 55% of the deaths were attributed to synthetic opioids, such as fentanyl. In 2019, a SAMHSA survey found that only 18% of the 1.6 million people with opioid-use disorder received medication assisted treatment.
New Problems
The legalization of medicinal- and recreational-use marijuana in 17 states has unleashed new substance use problems among the elderly, Blow said.
“It’s important to remember that cannabis is much more potent than it was 10 years ago. Overall, its use among the elderly has risen from 2.9% to 9.6% in 10 years,’’ Blow said. “The trend among the elderly is an increase in the use of edibles.’’
Risks in cannabis use include short-term memory loss, depression, impaired cognition, impaired motor coordination, and cannabis-dependency, Blow said.
“Mental illness is twice as prevalent with cannabis users as among non users,’’ Blow said. “The old, about 33%, don’t tell their doctors they are using, and 21% of older cannabis users don’t have a doctor.
“It’s the Wild West about medical cannabis and the Alzheimer’s and dementia effect.”
— Frederic C. Blow, University of Michigan Addiction Center
“We don’t know if cannabis use and some medicine-use combinations are dangerous. We should pay attention to this. It’s the Wild West about medical cannabis and the Alzheimer’s and dementia effect. There are not enough studies on cannabis use yet to know if it helps or hurts.’’
Treatment for substance use disorders must begin, Blow said, with this reality: “You have to meet the old where they are!’’
Finding Help
Blow said that SAMHSA’s TIP 26 recommends screenings, followed by brief interventions, and treatment.
He recommended several government and private programs for clinicians that offer guidelines and protocol for treatment. Included were SAMHSA’s TIP 26 project; the Florida BRITE Project; the National Institute on Alcohol Abuse and Alcoholism (NIAAA), and the Center of Excellence for Behavioral Health in Aging.
“Do not say alcoholic and don’t say problem drinker: Say we think you’re drinking over the mandated limits. Certain words can be very stigmatizing for an individual and by using certain terms you can trigger resistance. The older are very fearful to be labeled a problem drinker,’’ Blow said.
In order to counsel and treat substance disorders among the elderly, he said, “it’s important to find out what they use and to what extent.
“Yes, you can ask a direct question! But focus on the medical and the health aspect; don’t use stigmatizing terms. Imbed the session in medical questions, and routinize the questions. Providers need skills to treat abuse.
“These sessions can be done in any setting, but the older like the home or clinic setting, a residential setting. It’s motivation enhancement,’’ he said.
The government’s telecommunications service, Telehealth, which offers virtual medical help for substance disorders, has proven to be a popular treatment tool with older patients, Blow said, especially during the COVID pandemic. Providers include the Hazelden-Betty Ford Foundation’s RecoveryGo service, which includes counseling and treatment for substance and mental health disorders.
Additional Questions
Eric Weakley of SAMHSA presented questions from the online audience. One question asked if self-help groups Alcoholics Anonymous and Narcotics Anonymous are effective in treating substance disorders.
“Yes,” replied Blow. “There is no wrong door; they are not for everyone but they are lifesaving for many adults.’’ He was also asked whether risk-reduction programs are effective.
“Risk reduction can be very powerful to those who can’t change their behavior and want to keep drinking,” said Blow. “There are a number of programs for mutual aid/group reduction that encourage the health aspects. Reduction is controversial in the United States, which promotes abstinence, so proceed with caution.’’
In a four-decade career in journalism, Eleanor O’Sullivan has reviewed many books on best practices for financial advisors, has written for Financial Advisor and the USA Today network, and was movie critic for the Asbury Park Press.