If your clients aren’t listening to your advice, chances are they may not be hearing it.
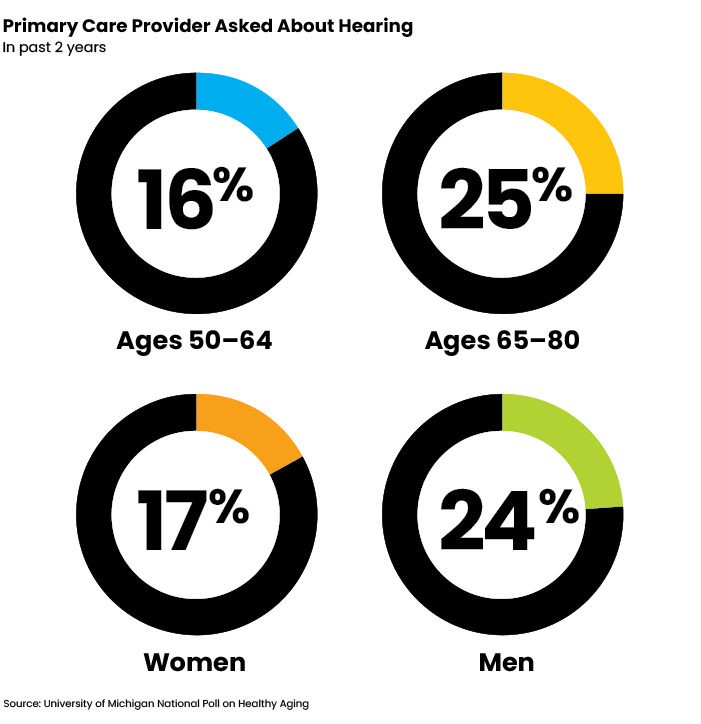
Only 16% of adults age 50-64 and 25% of adults age 65-80 report that their primary care provider has asked about their hearing in the past two years, according to results published this month from the University of Michigan National Poll on Healthy Aging. The poll, conducted in June 2020 and co-sponsored by AARP and Michigan Medicine, the university’s academic medical center, was based on responses from a national sample of more than 2,000 adults age 50-80.
According to the poll, men were more likely than women to report being asked about their hearing (24%, compared with 17%). Approximately just one in four older adults (23%) said they had a hearing test by a health care professional in the past two years, with the results again skewing more towards men (28%) than women (18%).
In total, 16% of the adults polled said they had fair or poor hearing. That percentage rose to 28% among those in fair or poor physical health and 31% for those in fair or poor mental health. Older adults in poorer physical or mental health were also less likely than those reporting better health to have had their hearing tested in the past two years.
Meanwhile, just 6% of the poll respondents reported using a hearing aid or cochlear implant, although “numerous studies show that at least 50% of adults probably have some degree of hearing loss,” noted a press release highlighting the results of the poll.
“Many people don’t realize they’ve lost hearing ability unless they’re screened or tested,” Michael McKee, M.D., M.P.H., a family medicine and health services researcher at Michigan Medicine, said in the release. “Age-related hearing loss can have wide-ranging consequences,” and could be addressed with assistive technology if that loss is detected.
Older adults’ hearing loss can contribute to poorer health, reduced quality of life and social isolation. Research also shows that individuals with impaired hearing are also at increased risk for dementia and falls.
McKee and Philip Zazove, M.D., chair of Michigan Medicine’s Department of Family Medicine, helped develop the questions and analyze the results in the poll report. The doctors, who use cochlear implants, stress the importance of hearing-loss diagnosis, proper intervention and adequate insurance coverage.
Health insurance plans vary widely in the coverage they offer for hearing screenings by primary care physicians, hearing tests by audiologists, hearing aids and cochlear implants, Zazov noted in the release, which also stated that:
• Traditional Medicare doesn’t cover routine hearing tests or devices but encourages primary care providers to use standard questionnaires about hearing during annual wellness visits.
• Medicare Advantage plans and employer-based insurance plans may cover some hearing-related services, while Medicaid coverage varies by state.
• Veteran Affairs health coverage is mainly for hearing issues tied to military service.
The COVID-19 pandemic has further stalled implementation of the Over-the-Counter Hearing Aid Act of 2017, which would let patients bypass doctor appointments and purchase much less expensive OTC hearing advices, which would be regulated and approved by the U.S. Food and Drug Administration.
Nearly two-thirds (62%) of those responding to the National Poll on Healthy Aging said they feel it’s somewhat or very important to have hearing tests every two years. So encourage your clients to get their ears checked — and speak louder and clearer.
Jerilyn Klein is editorial director of Rethinking65.







